Health Claim Administrators: A Look at Client Services
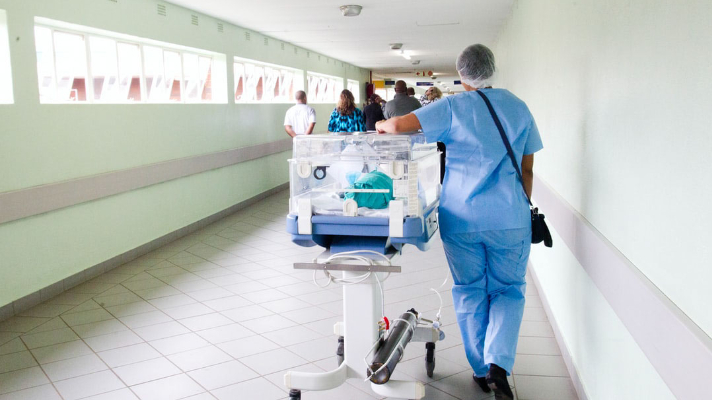
The recent increase in urgent care facilities and walk-in clinics has greatly increased the need for efficiency in the area of client services. Group health providers are now able to offer client services in a capacity that streamlines the administrative process for patients when they are in urgent care and walk-in clinics. Here’s a look at some of the ways that provider services utilize third-party administrative help services, such as health claim administrators, to be of direct benefit to patients.
Customer Service
Having a health claim administrator who can deal directly with customer service issues in a walk-in or emergency urgent care clinic is one way to make sure that matters that arise are taken care of efficiently. It is virtually impossible for the staff of a facility such as a walk-in to oversee customer service matters in addition to all the other responsibilities that they are handling. This is because the very nature of customer service matters often requires repeat phone calls and being passed along in a chain of administrators. Also, having one individual as the contact person makes the process go much smoother since it helps avoid repeating information over and over.
Third-party administrators are key conduits in customer service matters.
Claims Analysis
The area of claims analysis is intricate, to say the least. It seems that it is getting more complex on a daily basis. As the demographics change, the data associated with plan analysis also changes. This requires an individual who can keep up with these demands. For instance, one must be able to handle data associated with insured and uninsured claims as well as other programs. This is a very fluid topic; percentages increase and decrease every year. For example, there was a decrease in the percentage of people covered by Medicare between the years 2017 and 2018 of nearly 10%; the number of people covered fell to a total of 17.9%, dropping by 0.7%. Tracking and analyzing this data is crucial to efficient claims analysis.
Legal Counsel
Access to legal counsel is a critical need for services offering or providing medical treatment and/or referrals. Having this resource is an indispensable advantage which third-party health administrators are able to provide. The presence of legal counsel protects owners, employees, and clients equally.
Claims Processing
Provider services which offer claims processing alleviate much of the paperwork associated with running an urgent care. Health claims administrators handle the processing of claims efficiently. In addition, having a third-party individual process the claims could reduce the possibility of errors that might occur from medical staff processing paperwork claims in addition to all their other responsibilities. Overall, this benefits both clients and owners as well.
Recap: Client Services and Today’s Third-Party Administrators
In addition to handling client services to make the process for patients more efficient, a group health provider organization is also able to assist the owners of the urgent care walk-in facility with in-house administrative details. Third-party administrators do this by overseeing employee benefits such as flexible spending accounts and retirement accounts, for instance. Using a third-party administrator to handle and process claims and paperwork is often as cost-effective as doing the same work in-house. Thus, the client services and the administrative paperwork are all taken care of by professionals. This creates a win-win for everyone – patients, employees, and owners.
